(440) 600 7675
(440) 771 1731

Venous Disease
Over thirty million people in the United States are affected by venous disease, a chronic and progressive condition. Normally, veins return blood to the heart and lungs so that it can oxygenate and then bring that oxygen to all the tissue, muscles, and organs in the body. In order for veins to fight gravity and carry the blood in the correct direction, the valves within the veins must function properly. Factors such as age, pregnancy, family history, and lifestyle can cause these valves to weaken over time. When valves malfunction, blood collects in the veins of the lower extremities, leading to the development of varicose and spider veins.
Vein Disease Symptoms
Below is a list of symptoms associated with venous disease, though many people have none and seek treatment for cosmetic reasons. We are happy to help make your legs look and or feel better. At Solon Vein Clinic, we will work with you to develop a treatment plan personalized for your legs!
Aching/pain
Cramps
Heaviness
Itching
Burning
Throbbing
Leg fatigue
Restless legs
Swelling
Skin changes or discoloration
Ulcers
Bleeding varicosities
Vein Disease Conditions
Chronic Venous
Insufficiency
Veins have one-way valves inside of them that allow blood to travel back to the heart. Over time, these valves can weaken and malfunction, causing blood to pool in the veins. These distended, tortuous veins are called varicose veins and may cause symptoms described below. This process is known as chronic venous insufficiency.
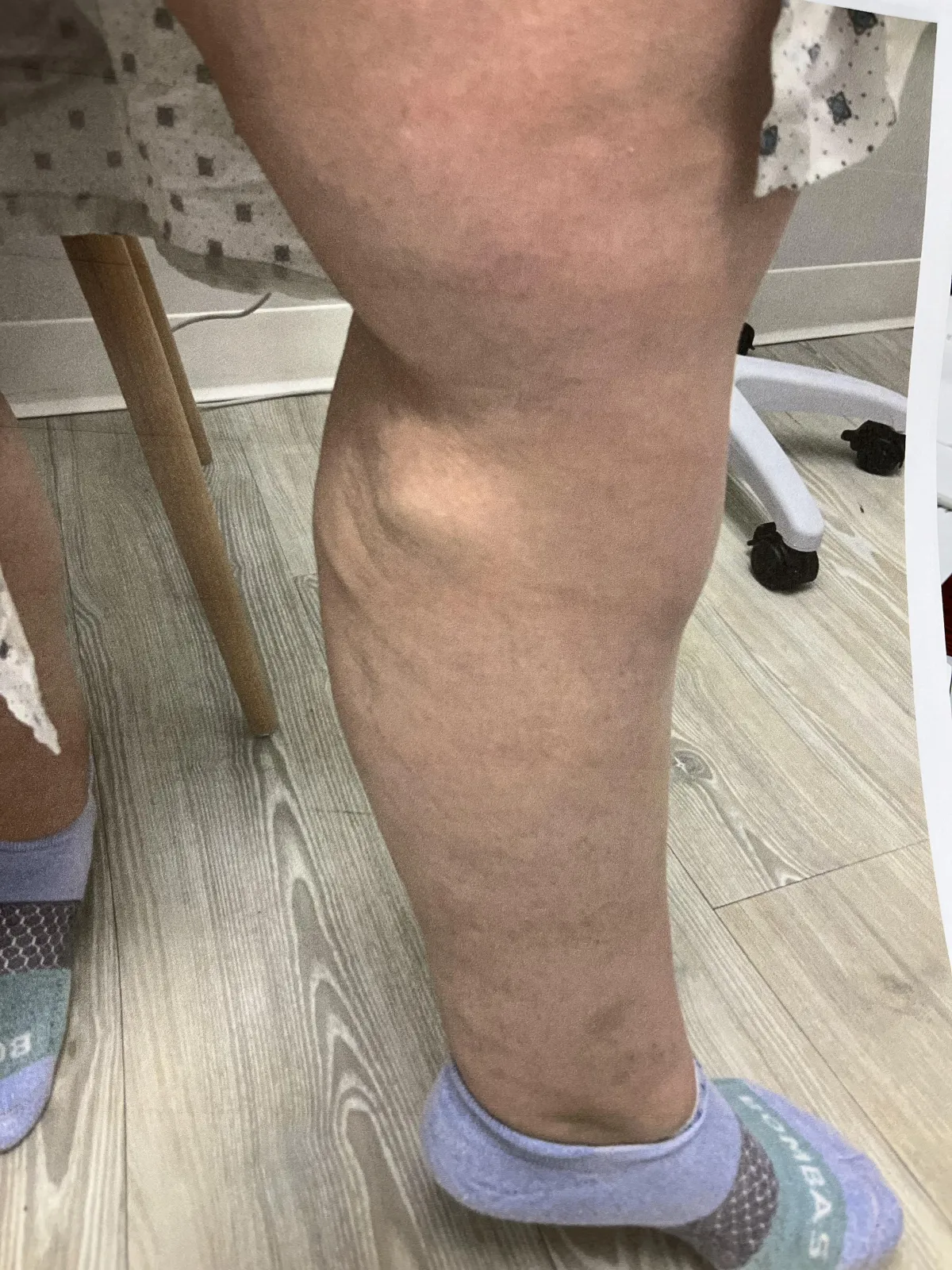
Symptoms
Swelling, heaviness, aching, pain, cramping, restless legs, skin changes, skin discoloration, varicose veins, or leg ulcers.
Risk Factors
Genetics, pregnancy, obesity, age, long periods of sitting or standing, injury to the legs, history of blood clots.
Treatment
The initial treatment for chronic venous insufficiency is usually conservative treatment that you can try at home. This includes wearing compression stockings to improve circulation, elevating your legs, and exercising regularly. If these measures are ineffective, an ultrasound of your legs may be necessary to diagnose reflux, or the backflow of blood, in your larger superficial veins. Your provider will work with you to determine the best treatment option for you.
Deep Vein
Thrombosis
The body has a superficial and deep system of veins. Veins that you can see and become varicose veins are part of the superficial, whereas the deep system does the majority of pumping blood back to the heart. Deep vein thrombosis, or DVT, is a blood clot that forms within the deep veins and can be diagnosed with an ultrasound. It is a concern because a clot in then deep system of veins can travel to the heart, lungs, and brain. This puts the body at risk for a heart attack, pulmonary embolism, or stroke.
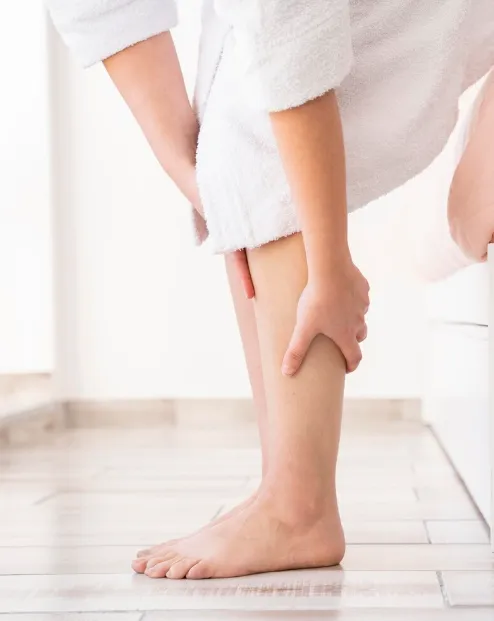
Symptoms
DVTs can be asymptomatic, however, typically a person with a DVT experiences redness, swelling, pain, and warmth to the area.
Risk Factors
Prolonged immobilization or bedrest, age over 40, recent surgery, obesity, smoking, certain types of cancer, clotting disorders, varicose veins, and pregnancy.
Treatment
Deep vein thrombosis can lead to serious complications if left untreated. If you are diagnosed with a DVT, you will be prescribed a blood thinner and be closely monitored with further ultrasounds.
Lymphedema
The lymphatic system is responsible for removing waste and excess fluid from tissue all over your body. It is an important part of your immunity and keeping you healthy. When a blockage occurs or there is damage to the lymphatic system, it can cause a buildup of lymph fluid, or lymphedema.
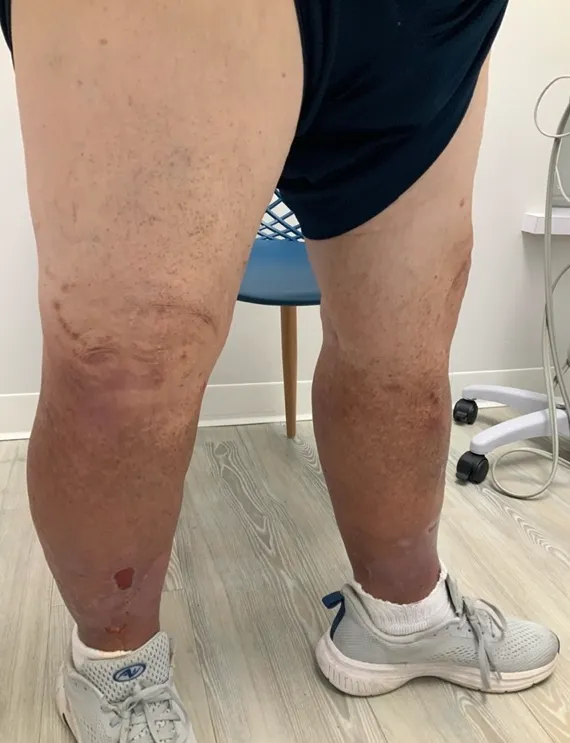
Symptoms
Swelling of one or both legs.
Treatment
Treatment will be based on the severity of the disease and can include compression stockings, pneumatic compression, manual lymph drainage, or complete decongestive therapy. At Solon Vein Clinic we can help diagnose and treat this condition and obtain the ancillary treatment that may be needed.
Superficial
thrombophlebitis
Thrombophlebitis is the inflammation of a vein, usually secondary to the formation of a blood clot in a superficial vein.
Because the affected vein is located in the superficial system, there is a much lower risk of the more severe complications that occur with deep vein thrombosis. A sedentary lifestyle, smoking, obesity, pregnancy, and certain medications can put you at increased risk for developing blood clots.
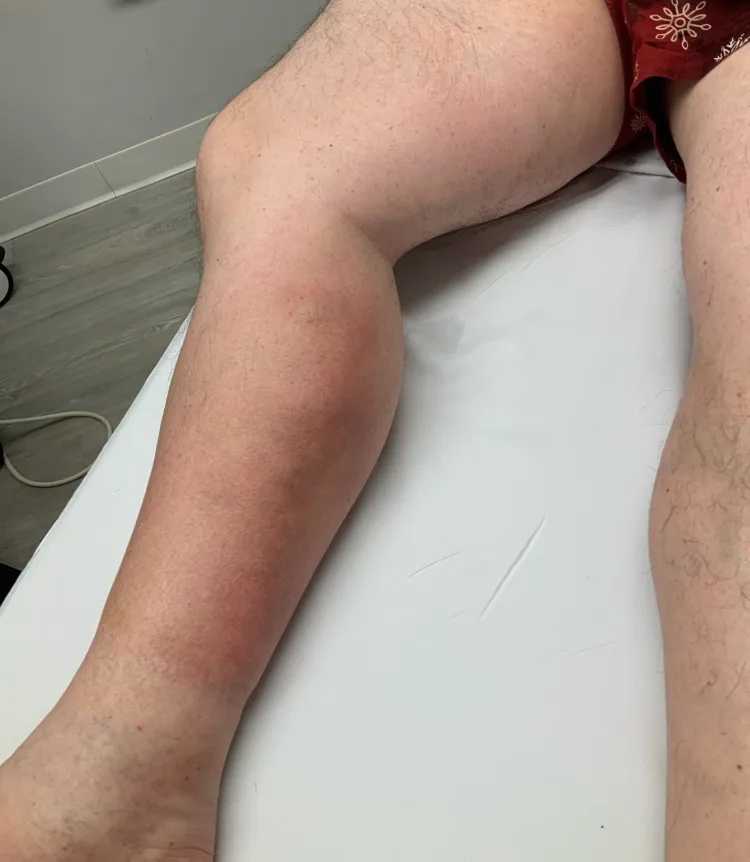
Symptoms
Redness, warmth, tenderness, itching, and swelling.
Treatment
The main management in uncomplicated cases is based on local heat, compression stockings and antiinflammatory medications. In some cases, surgical procedures may be necessary.
Post-Thrombotic
Syndrome
Post-thrombotic syndrome (PTS) can develop after a deep vein thrombosis. The previous clot causes inflammation and damages the valves, affecting the adequate venous blood flow. When blood flow is blocked, it increases intravenous pressure and causes blood to collect in the affected leg.
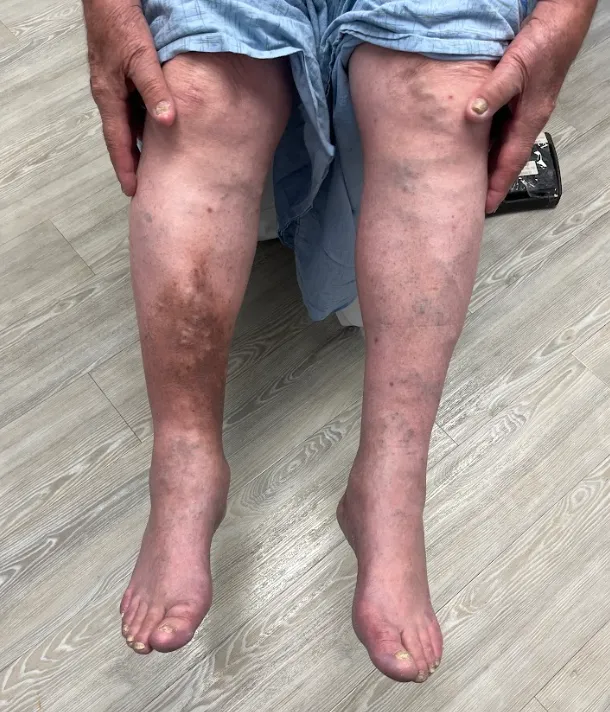
Symptoms
Leg pain, swelling, cramping, heaviness, dry/flaky skin, difficulty walking or standing, changes in skin pigmentation and ulcers (wounds).
Treatment
Unfortunately, there is no simple way to replace or repair damaged valves. However, non-invasive conservative therapy can help with the symptoms and reduce the risk of complications.
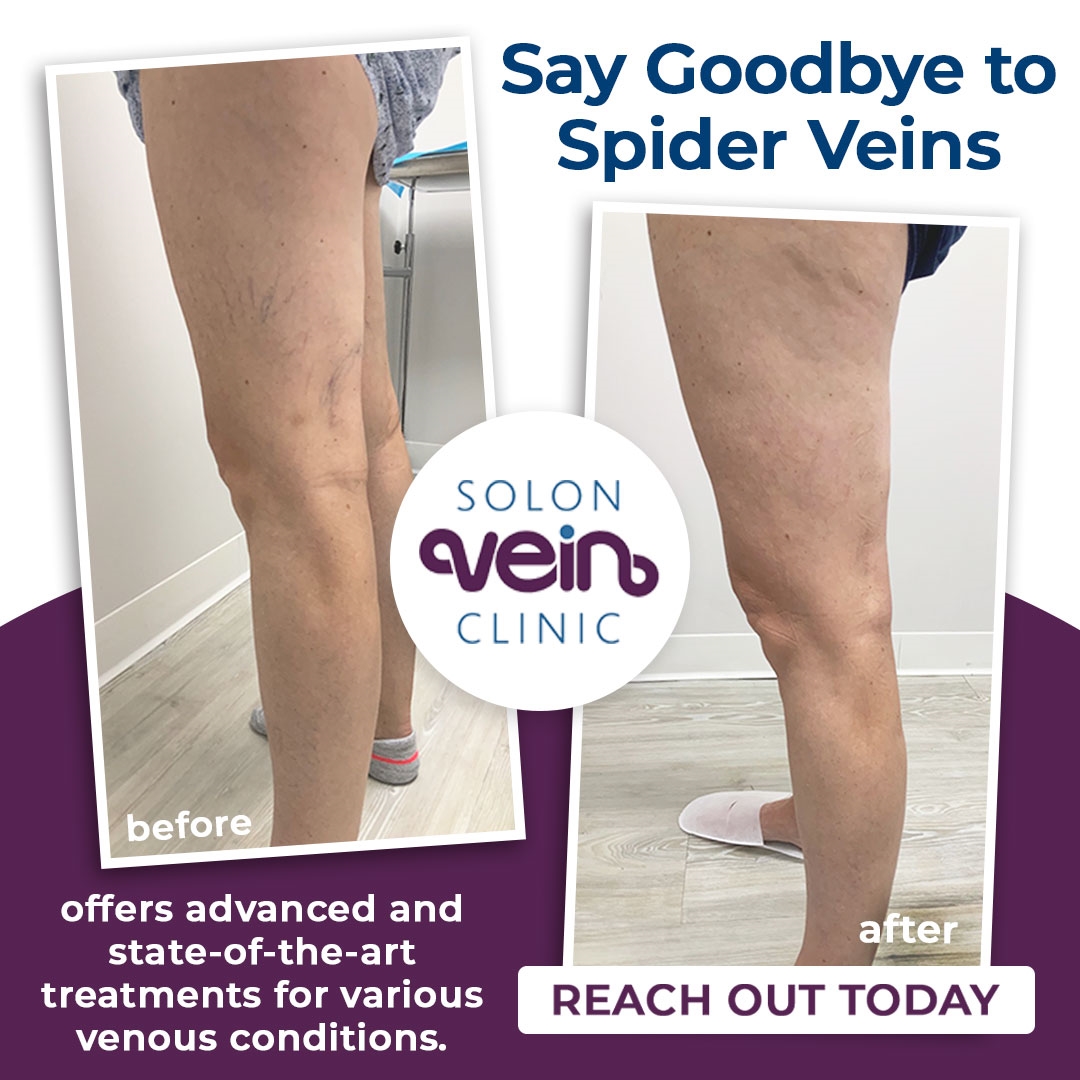
Spider Veins
Spider veins are small, dilated blood vessels close to the surface of the skin. They usually appear red, blue, or purple in color and can look like a bruise that doesn’t heal. They are more frequently seen in the legs, but could affect different parts of the body like chest, breast, back and others. You may have an increased risk for developing spider veins if you have a family history of spider or varicose veins, have been pregnant, are overweight, or spend extended periods standing or sitting.
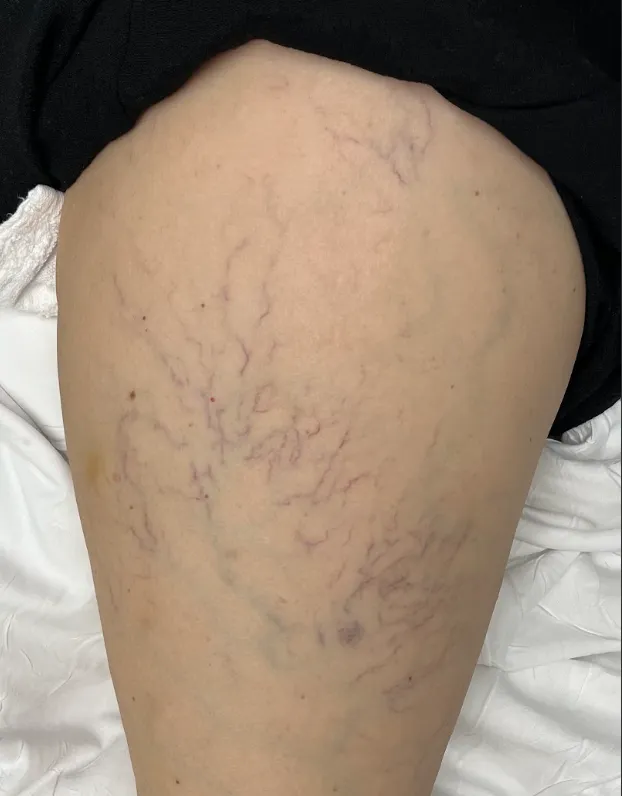
Symptoms
Pain, aching, burning, itching, or they may be asymptomatic.
Treatment
Whether or not your spider veins are symptomatic, they can be treated with injection sclerotherapy or laser treatment.
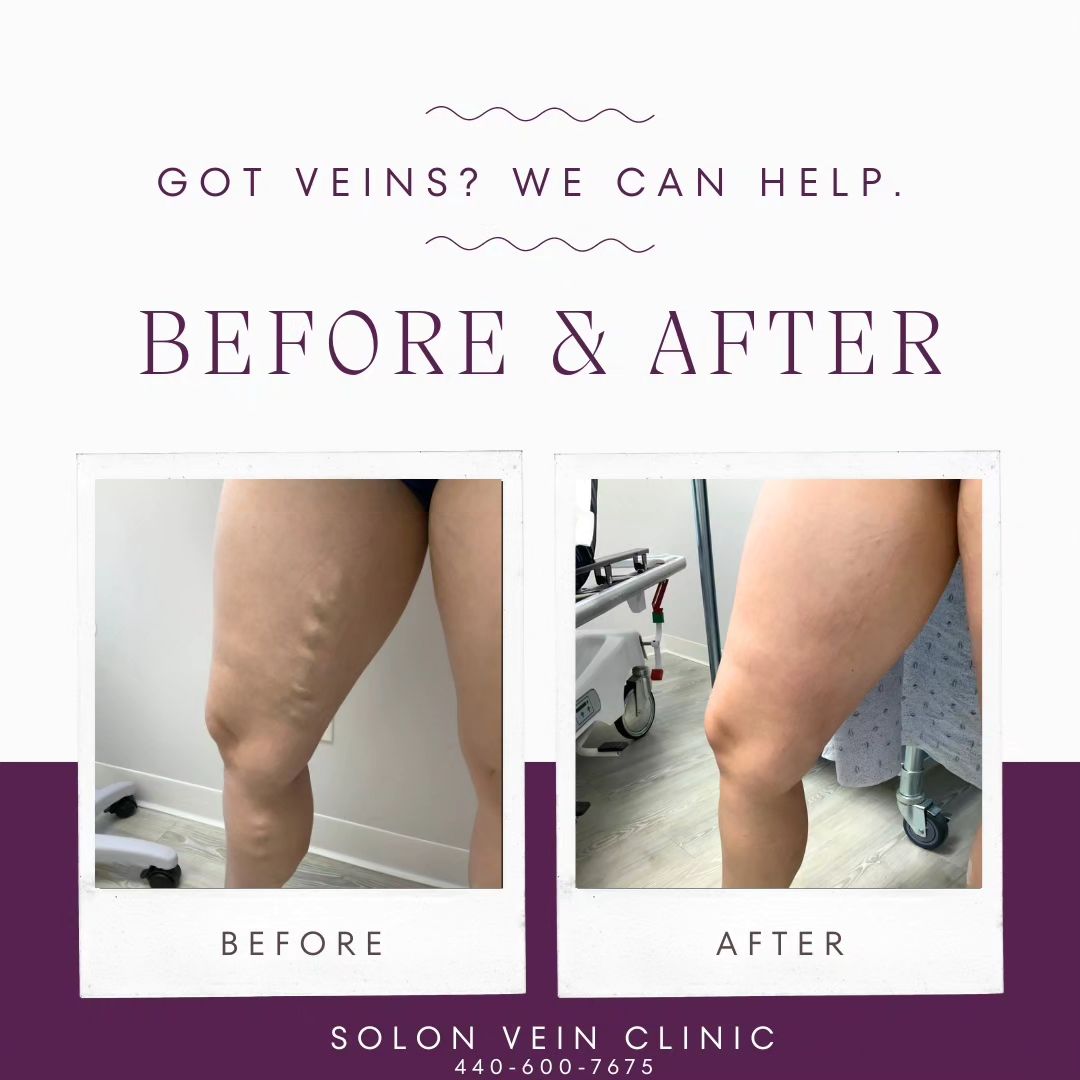
Varicose Veins
Varicose veins were once healthy and a normal size, but they become distended (bulgy) over time. This typically happens when the valves in your veins weaken and cause blood to backflow and collect in the vein. Varicosities are veins that are larger than normal, blue or green, tortuous, and may protrude through the skin. The same risk factors for spider veins put you at risk for developing varicose veins including gender, age, weight, family history, and lifestyle.
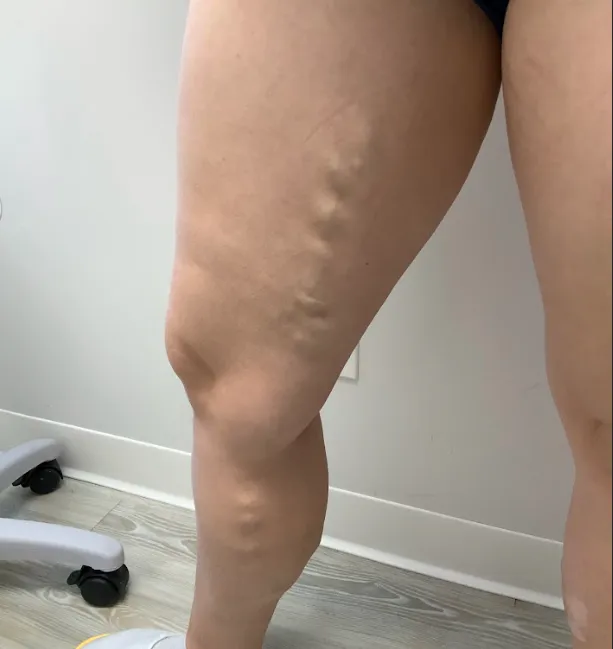
Symptoms
Large bulging and twisting veins, cramping, aching, pain, heaviness, leg fatigue, and swelling.
Diagnosis and treatment
Your varicose vein symptoms can be improved with conservative measures like compression, elevation, weight loss, and exercise. However, invasive treatment offers the possibility of more significant and permanent symptom improvement and a better cosmetic appearance. Treatment will depend on your symptoms, and the location, size, anatomy, and pathophysiology of your veins.
Venous Reflux
In a healthy circulatory system, blood in the veins flows in one direction, back to the heart. Valves make this happen by closing within the veins and preventing gravity from pushing blood backwards. When valves weaken over time, they do not close completely to prevent reflux and blood from pooling in the vein. Venous reflux can cause veins to become larger than normal and take up extra space in your legs, resulting in many of the symptoms below.
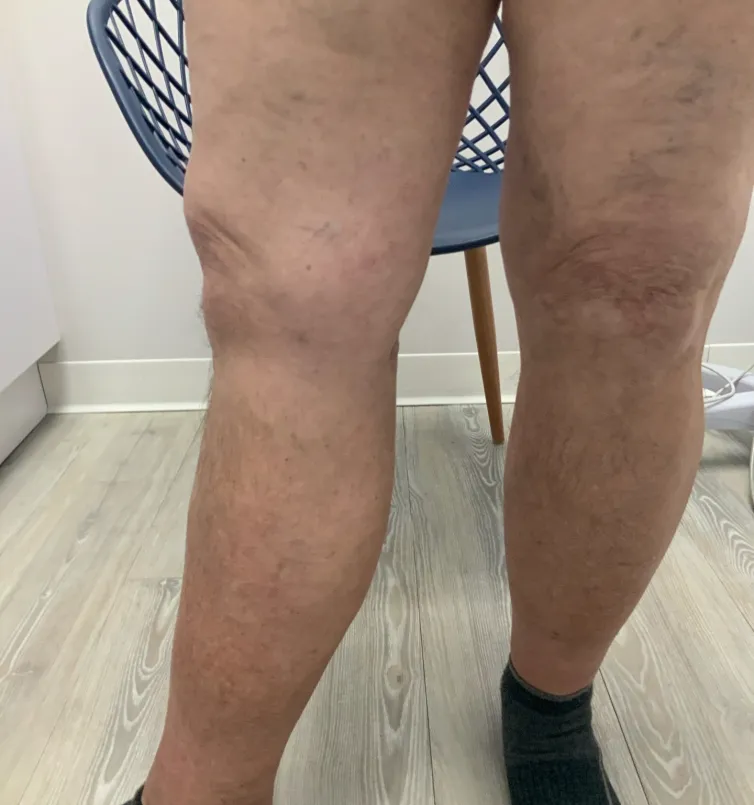
Symptoms
Cramping, heaviness, leg fatigue, restless legs, swelling, and varicose veins.
Diagnosis and treatment
A special type of ultrasound of the veins will help to diagnose venous reflux by assessing the size of the veins as well as the amount of reflux (abnormal backflow). Depending on the results of your ultrasound, the staff at Solon Vein Clinic will help to create a treatment plan to improve your symptoms. This may include medical management and minimally invasive therapy when necessary and indicated.
Venous Stasis Dermatitis
Venous stasis dermatitis is a skin condition that develops when poor circulation in the legs causes blood to pool in the veins. Increased pressure in the veins allows fluid and blood cells to leak into surrounding tissues, leading to inflammation and changes in the skin. Over time, this chronic venous insufficiency can cause the skin to become fragile, irritated, and more prone to infection or ulceration if left untreated.
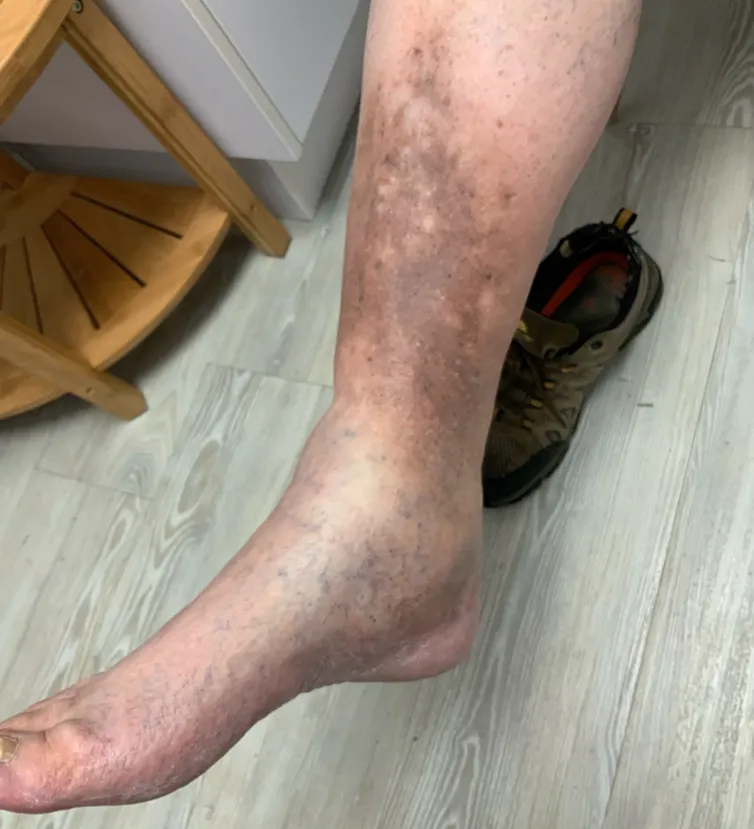
Symptoms
Open sores near the ankles, pain or aching in the legs, swelling, skin discoloration, drainage from the wound, and slow or poor healing. Ulcers can get infected and compromise limb function and life.
Diagnosis and treatment
Diagnosis typically includes a physical exam and an ultrasound to evaluate underlying venous disease. Treating the root cause of poor circulation is essential to managing venous stasis dermatitis. Depending on severity, treatment may include compression therapy, topical medications to reduce inflammation, and minimally invasive vein procedures such as ablation or VenaSeal to improve blood flow and prevent progression.
Venous Ulcer
A venous ulcer is an open wound that develops when prolonged venous insufficiency prevents blood from flowing properly back to the heart. Increased pressure in the leg veins damages surrounding tissue, causing the skin to break down and form a slow-healing wound, most commonly around the ankles. Without proper treatment, venous ulcers can become chronic and significantly impact mobility and quality of life.
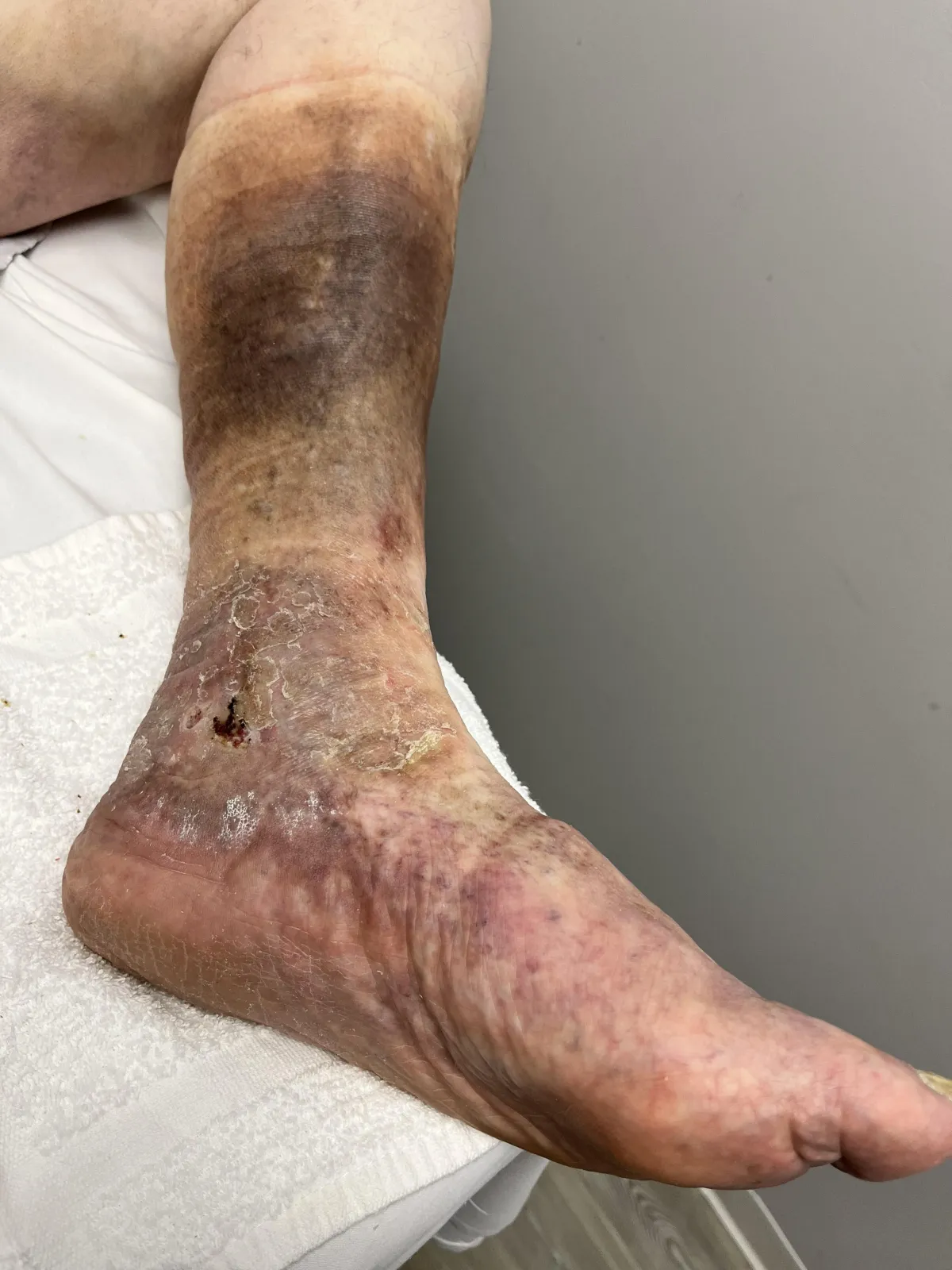
Symptoms
Open sores near the ankles, pain or aching in the legs, swelling, skin discoloration, drainage from the wound, and slow or poor healing.
Diagnosis and treatment
Diagnosis usually includes a physical examination and an ultrasound to assess underlying vein disease. Effective treatment focuses on improving circulation and promoting wound healing. This may include compression therapy, wound care, and minimally invasive vein treatments such as ablation, Varithena, or VenaSeal to address the underlying venous insufficiency and reduce the risk of recurrence.
TESTIMONIALS
CONTACT US
440-771-1731
Monday-Friday: 8:30 am - 5:00 pm
Saturday & Sunday: CLOSED
33290 Bainbridge Rd Solon, OH 44139